The Procedure
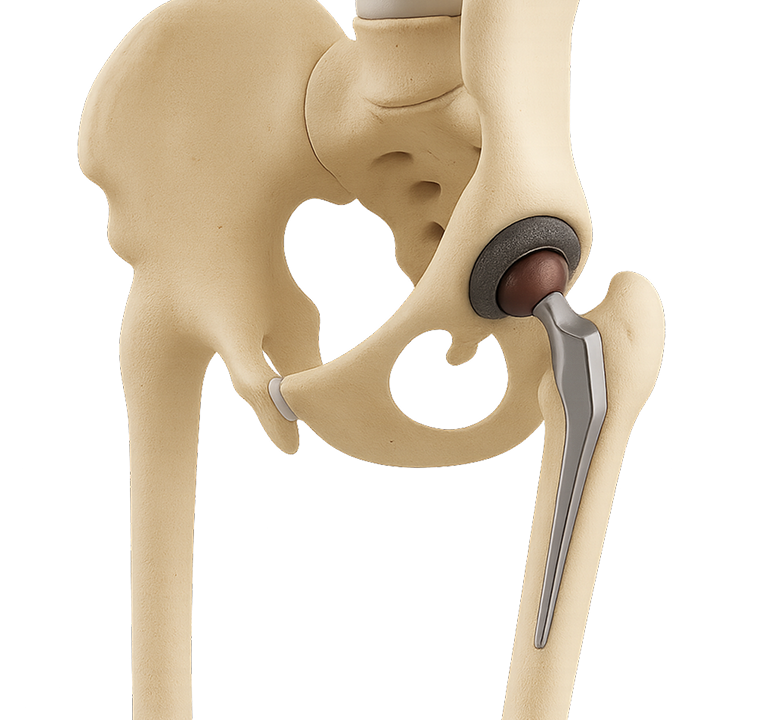
The hip is a ball-and-socket joint where the round head of the femur moves within the acetabulum, the socket that holds the ball in place. This socket is lined with the labrum, a rim of cartilage that stabilizes the joint, which itself is encapsulated by the synovial membrane. Due to the complexity of this joint, a range of problems can arise in the hip, necessitating advanced diagnostic and treatment methods, such as hip arthroscopy.
Hip arthroscopy is a minimally invasive surgical procedure performed to diagnose and treat a variety of hip problems. Common indications for hip arthroscopy include:
● Labral tears, which is when the cartilage lining the hip socket gets torn;
● Femoroacetabular impingement (FAI), when the ball of the hip joint impinges on its socket;
● Damage to the ligamentum teres, the ligament connecting the ball and the socket of your hip;
● Synovitis, an inflammation of the membrane lining your joint due to various diseases.
Your surgeon may recommend hip arthroscopy if you experience persistent hip pain, restricted motion, or mechanical symptoms such as catching or locking that do not respond to non-surgical treatments.
During the surgery, the surgeon makes small incisions around the hip joint and inserts a camera (arthroscope) and specialized instruments to visualize and treat the problem. The arthroscope transmits images to a monitor, allowing the surgeon to guide the instruments to repair or remove damaged tissues. The procedure typically takes between one to two hours, depending on the complexity of the condition being treated.
Risks and Complications
Hip arthroscopy is generally considered a safe procedure, but like all surgeries, it carries risks. As expected from a minimally invasive procedure, the risks of a complication arising from a hip arthroscopy are quite low (0.58%), although still present, and mainly consist of:
● Injury to the cartilage or labrum
● Nerve injury
More serious but even rarer complications include:
● Hip dislocation
● Fracture of the hip
● Necrosis of the hip
● Heterotopic ossification (excessive bone growth often in response to injury)
● Infection of the joint
General minor risks of surgery and anesthesia include nausea, vomiting, headaches, sore throat, and urinary retention. General major risks include blood clots, which can lead to heart attack or stroke, allergic reactions, infection of the surgical wound, and pneumonia. Your surgeon will make sure to discuss the relevant risks with you prior to your surgery and take precautions to minimize the risk of any complications.
What to Expect
Before the procedure, your surgeon will ensure a thorough pre-surgical workup is done. This typically includes a physical examination of your hip, blood tests, and imaging studies such as X-rays or MRI to better visualize your joint.
The most common type for hip arthroscopy is general anesthesia, but regional anesthesia (e.g. spinal, epidural, nerve block) may also be an option.
After the procedure, your surgeon may prescribe pain medication such as ibuprofen (e.g. Advil), acetaminophen (e.g. Tylenol), naproxen (e.g. Aleve) or opioids (e.g. oxycodone) for short-term pain management. Nerve blocks may also be used in some cases to provide immediate pain relief.
Your Recovery
After an outpatient hip arthroscopy, you can expect to go home on the same day as the procedure, provided your surgeon determines that your recovery is on the right track. You will receive instructions on the medications to take after your surgery for pain relief or blood clot prevention. Starting physiotherapy early will help prevent your hip from stiffening. Your physical therapist will guide you through a regimen designed to restore mobility and function; you can expect to begin light exercises and stretches immediately after the surgery. Your full recovery, including returning to sports or exercise, can be expected to last three to six months, although you should be able to drive safely as early as two to four weeks after your procedure. During your recovery, you should avoid high-impact activities such as manual labor, heavy lifting, and intense sports. Your surgeon will make sure to explain when you can resume your daily activities, and your follow-up appointments will ensure your recovery is on track.
